More folks recognize the need to safeguard antibiotics for future use, but we’re a long way from figuring out how. First of a six-part series investigating the future of antibiotics in beef production.
March 27, 2017
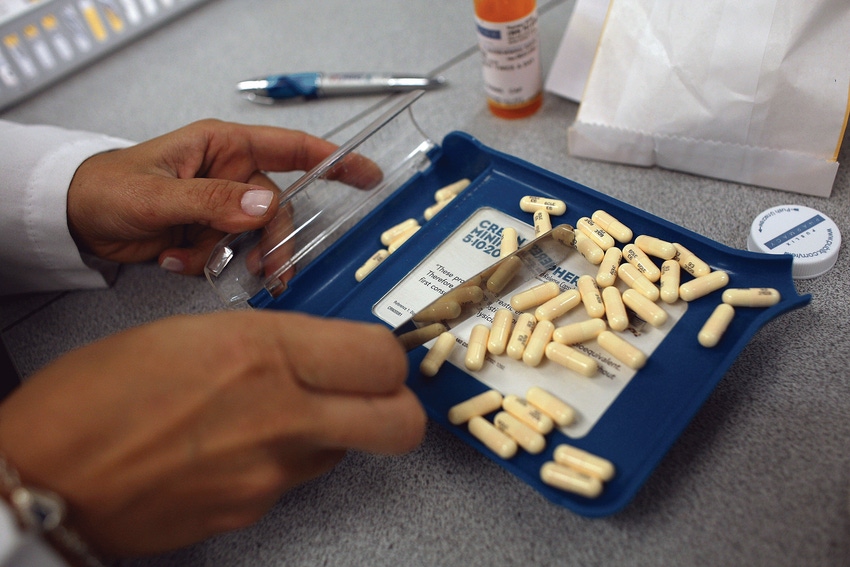
“We’re reaching a postantibiotic era where we have patients with infections that we can’t treat,” says Kurt Stevenson, a physician and medical director at Ohio State University. “Antibiotics are unlike any other drug, in that use of the agent in one patient can compromise its efficacy in another.”
Stevenson shared insights from the medical community at the Antibiotic Use Symposium hosted by the National Institute for Animal Agriculture (NIAA) last fall — the sixth in as many years.
Consider that The Food and Agriculture Organization of the United Nations estimated in November that approximately 700,000 human deaths each year are related to antimicrobial-resistant (AMR) infections. The toll on human health results in a vicious circle with economics.
“Drug-resistant infections have the potential to cause a level of economic damage similar to — and likely worse than — that caused by the 2008 financial crisis,” according to a September report from the World Bank titled Drug Resistant Infections: A Threat to Our Economic Future.
According to the report, in a high-case scenario, antimicrobial resistance could cause low-income countries to lose more than 5% of their GDP, and push up to 28 million people — mostly in developing countries — into poverty by 2050.
More broadly, according to the report — based on World Bank Group projections of the world economy for 2017-2050 — global GDP would fall by 1.1% in the low-impact AMR scenario and 3.8% in the high-impact AMR scenario. In 2050, the volume of global real exports would shrink by 1.1% in the low-case scenario, and by 3.8% in the high-case scenario. By 2050, the decline in global livestock production could range from a low of 2.6% to a high of 7.5% per year.
Growing challenge
So, while there remain more questions than answers about what contributes to human antibiotic resistance — and how much — there’s little debate that human antibiotic resistance is a growing challenge in the United States and around the world.

That’s also why, despite science and the tenuous causal relationship between antibiotic use in livestock and antibiotic resistance in humans, consumers continue clamoring for less antibiotic use in producing their food.
“Consumers care about this issue,” says Angie Siemens, vice president of food safety, quality and regulatory at Cargill. “You will continue to see the marketplace move, no matter what the science is, no matter what the metrics are, no matter what the regulations are.”
Speaking on a panel discussion at the NIAA symposium, Siemens described a number of initiatives undertaken by Cargill, including the company eliminating 20% of the shared-class antibiotics from eight feedyards, representing 1.2 million head of fed cattle in 2016. By 2018, she says 90% of the cattle Cargill harvests in the U.S. will come to them with Beef Quality Assurance certification.
Keep in mind, Cargill and similar companies are dealing with the issue in more countries than the United States; Cargill has 70 businesses in 67 countries, with food animal nutrition businesses in most of them.
“We know antimicrobial resistance is a global concern, and we want to be part of the solution,” says Christine Daugherty, vice president of sustainable food production for Tyson. “We also know that we cannot compromise animal well-being. If animals get sick, they need to be treated. We work with 11,000 independent farmers and ranchers to supply the material we need. These are individuals whose livelihoods depend on us and others providing consumers with a safe, wholesome product.”
Human and animal collaboration
At the NIAA symposium, veterans of the debate on the livestock side of the fence sensed a growing recognition from the human health community regarding the need to preserve antibiotics for livestock, too.
“From FDA’s perspective, we do recognize that antibiotics are not only important for treating disease, but that they’re important tools for preventing disease as well,” says Bill Flynn, deputy director for science policy at the Food and Drug Administration’s (FDA) Center for Veterinary Medicine. “In the spirit of the One Health idea [see next paragraph], I think the notion is that we need to look at all of the different uses in all of the different settings, whether it’s in various human health care settings or the various veterinary settings.”
If you’re unfamiliar with it, the One Health Initiative is a global effort aimed at forging collaborations between health care providers in both human and animal medicine — from physicians to veterinarians, dentists, nurses and other scientific health- and environmentally related disciplines. The notion is that more can be done and understood to the benefit of all through more transparent communication.
Consider that more than half of hospital patients receive antibiotics each year, according to Christopher Braden, a physician and deputy director of the Center for Disease Control and Prevention’s (CDC) National Center for Emerging and Zoonotic Infectious Diseases.
Braden shared antibiotic prescribing rates per 1,000 people for the United States in 2014. It ranged from 501 per 1,000 in Alaska to 1,285 per 1,000 in West Virginia. So, regional and cultural behavior is part of it.
“Estimates show that 30% to 50% of antibiotics prescribed in hospitals are unnecessary or inappropriate; more than 50% in outpatient clinics are unnecessary,” physician Nate Smith told symposium participants. He is director and state health officer for the Arkansas Department of Health.
Before pointing fingers at the doctors, understand that most of us have likely been part of the problem at various times. Perhaps this sounds familiar: “Doc, I’m sure it’s got to be a sinus infection, just phone in a prescription that we can pick up when we get to town.” Or maybe you demanded an antibiotic for a sick kid who was writhing in feverish discomfort, though the doc figured it was a virus.

“I do think we walked away with a collaboration across stakeholders,” Siemens says. “Different stakeholders have different ideas about what it means to have antibiotic stewardship, how impactful animal agriculture is on human medicine. What we did have was the ability to sit down and have a conversation, and try to understand how we can work together and do it consistent with a One Health goal. What we don’t share is how we’re going to get there.”
About the Author(s)
You May Also Like





