How To Prevent Foot Rot In Cattle
The clinical sign of foot rot — lameness — is a performance-robbing condition that seemingly comes on overnight, but such infections can be minimized.
September 11, 2014
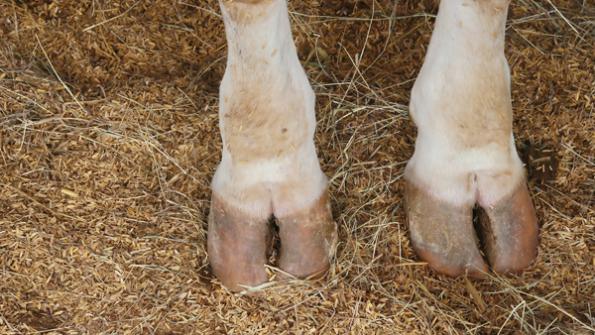
Foot rot is an infectious condition that causes swelling, heat and inflammation in cattle’s feet, resulting in severe lameness. Swelling and lameness can appear suddenly, with the animal walking normally one day but limping the next day. Lame cattle can lose weight quickly if they’re reluctant to travel to feed and water.
J. Dustin Loy, veterinary diagnostic microbiologist in the University of Nebraska’s Veterinary Diagnostic Center, says the microbes associated with foot rot are mainly anaerobes, meaning they thrive in an environment without oxygen.
“The most common is Fusobacterium necrophorum. We usually find one or more of several other anaerobic bacteria associated with it, including Prevotella and Porphyromonas. They’re all gram-negative anaerobes. We often find one that used to be called Arcano-bacterium pyogenes and is now called Truperella pyogenes. It forms pus and helps induce the anaerobic environment for other bacteria by reducing oxygen in the tissues,” he explains.

Andrew Niehaus
Andrew Niehaus, Ohio State University College of Veterinary Medicine, says the anaerobic bacteria are symbiotic. “One of them enters the break in the skin, and another comes along and helps perpetuate the infection,” he says. The bacteria multiply and further damage and destroy tissue, which leads to more anaerobic conditions as the tissue dies, which further facilitates the infection.
Many of these bacteria are normally found in feces. “The animals are always exposed to them, so there must be a predisposing factor such as a break in the skin — in the space between the toes,” Loy adds.
Once bacteria are introduced, it takes about a week for the bacteria to set up the anaerobic conditions needed to multiply rapidly and secrete toxins that cause tissue damage. Then the animal goes suddenly lame. The pain and lameness are due to immune responses that create inflammation and swelling.
Matt Miesner, clinical associate and a professor in Kansas State University’s College of Veterinary Medicine, says it’s hard to know why incidence varies from one year to the next. Perhaps it’s a variation in the pathogenicity of the strain of bacteria, but it may involve environmental factors.
“Maybe we had a wet spell and the feet become soft and more easily damaged. It doesn’t take much of an opening for bacteria to get started,” Miesner says. Just walking on gravel or sharp ice can create nicks and abrasions.
“Once you get a few cases, bacteria may be spread from draining lesions, putting a higher concentration in the environment. Once you have it, this tends to amplify it,” he says.
Kathryn Bach, a Colorado State University livestock intern, says foot rot may occur more frequently after a period of rain. “Cattle may congregate under shade trees where they defecate or urinate and their feet are wet,” she says. When tissue between the toes is softened by moisture or damaged by acid in manure, it’s more easily scraped or punctured.
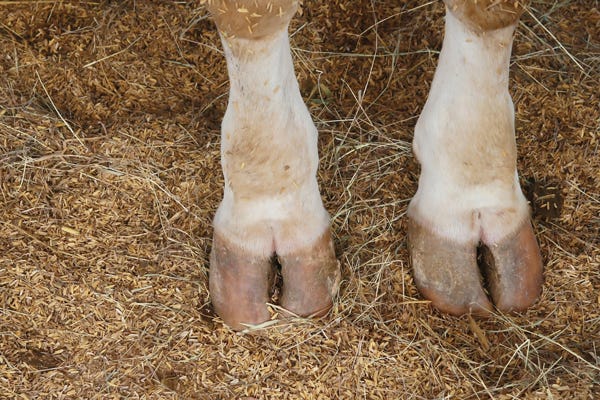
Make sure it's foot rot
Sometimes, foot rot is assumed because an animal suddenly becomes lame. While sudden, three-legged lameness is a classic sign of foot rot, it can also be due to fracture, snakebite, puncture, abscess or some other infection. “I’ve seen cattle with a rock or stick jammed between the toes reluctant to put weight on the foot,” Miesner says.
Examine the foot before administering antibiotics. “If the animal is in a chute for treatment, lift the foot with a rope to look at the bottom,” Niehaus suggests. “If you rope the animal on pasture, cast it to the ground for treatment and closer examination.”
Treating foot rot
Bach says several systemic products are labeled for foot rot, including Nuflor, Excenel, Naxcel, Draxxin, LA-200 and penicillin. Most organisms that cause foot rot are very responsive to antibiotics. Many people use long-acting oxytetracycline or Procaine penicillin because they’re less expensive, saving the big guns for more serious problems.
Pain is a major factor in foot rot, and may result in reduced feed and water intake in affected animals because walking is painful. Thus, producers should seek the advice of their herd health veterinarian to determine the best pain management options for their operation.
“The treatment I prefer is to lift the foot and use a strip of gauze soaked with Betadine to floss between the toes,” Miesner says. “This clears away the buildup of dead tissue and opens it to the air, which inhibits bacteria that love anaerobic conditions.”
Systemic antibiotics generally work well if the infection is caught early. “If infection is longstanding, you may have to clean up the foot — floss between the toes with clean rope, twine or a towel to remove necrotic tissue — and apply a topical antibiotic such as oxytetracycline,” Niehaus says. “Putting LA-200 on a gauze pad and wrapping the foot to hold it next to the affected area may help.” This also decreases shedding of bacteria into the environment.

Matt Miesner
“If the animal isn’t greatly improved within 3-4 days after antibiotic treatment, I look for some other cause of infection and lameness, or see if it’s gone into deeper tissues,” Miesner says.
Some cattle recover from lameness within a few days without treatment. “It has a lot to do with the animal’s immune status, how many bacteria got in initially, and how quickly the immune response can stop the proliferation,” Loy says. “The longer you wait, the longer the course of treatment that may be needed, but most of these bacteria are susceptible to the approved drugs for foot rot.”
Wait too long to treat, and systemic drugs might not be as effective, and the infection can move into the joint and cause permanent damage, which may necessitate surgery. “This might include removing all the dead tissue and cleaning it up so it can heal. Toe amputation would be the most drastic measure, if the infection has affected the ligaments and bone,” Bach says. Once these structures are damaged, systemic antibiotics are rarely helpful.
“If you have a steer or cull cow with bone involvement that you are trying to get to market, removing the affected toe will allow time to heal enough to get to market. This isn’t a long-term fix, but it might enable the animal to regain lost weight. Your veterinarian can help you decide whether this is worth doing,” she says.
“Some chronic cases that are hard to clear up may be caused by what some producers call super foot rot — bacteria resistant to antibiotic treatment. These are very difficult to treat, and you need to work with your veterinarian. Together, you can decide if you want to go to a salvage procedure, such as toe removal, or if the animal is beyond treatment,” Bach says.
Some prevention basics
“When cattle are on pasture, rotate them around so they’re not always congregating under the same trees every day,” Bach says. “Moving them to different areas alleviates manure buildup. Even moving feeders, mineral tubs, etc., can help.” The goal, she says, is to keep the environment as clean and dry as possible, and footing abrasion-free. In feedlots, mounds enable cattle to get out of the mud and help keep feet healthy.
“There aren’t many feed additives we can use for prevention, except zinc, to try to keep feet healthier. Zinc is one of the trace minerals important for hoof-horn growth,” Bach says. “Zinpro has done some research indicating some increase in daily gains and decreased incidence of foot rot with zinc added to the diet. The increased daily gains may not be directly due to addition of zinc, but zinc has been shown to help with skin and hoof health and integrity.”
Subscribe now to Cow-Calf Weekly to get the latest industry research and information in your inbox every Friday!
Meisner calls attention to feed-through antibiotics (oxytetracycline and chlortetracycline) labeled for preventing foot rot. If a veterinarian or producer anticipates issues with foot rot in certain situations, the practice might merit consideration if the cattle are in a feedlot. Isolating affected animals until the infection resolves will help prevent spread of bacteria in the environment.
“There are vaccines against Fusobacterium necrophorum as a preventive against liver abscesses and foot rot in feedlot cattle. Feedlots that use vaccine to try to limit incidence of liver abscesses generally see reduced incidence of foot rot. My experience is that vaccination may help reduce foot rot problems, but won’t eliminate them,” Miesner says.
Digital dermatitis on the rise
Papillomatous digital dermatitis (DD) is called strawberry foot rot, hairy heel warts and bovine digital dermatitis. Whatever the tag, it spells trouble.
DD is caused by a spirochete bacterium — Treponema spp. — and the lesion that appears with this type of lameness is a red, rough ulcer. It looks granular (like a strawberry), may have long hair-like structures growing from the heel, and is very painful, says Miesner.
DD can appear when any bovines are housed in groups or confined in a contaminated environment. “If a lame animal has a lesion between the toes or heel bulbs that looks like foot rot but doesn’t respond to antibiotics, a closer look may reveal its true nature,” Miesner says.
The disease doesn’t respond well to systemic antibiotics. “We usually use formalin foot baths, thoroughly rinsing the feet with an intensive program to try to halt the infection. We may use topical oxytetracycline spray and try to dry the foot. Moisture allows these bacteria to keep going,” he says.
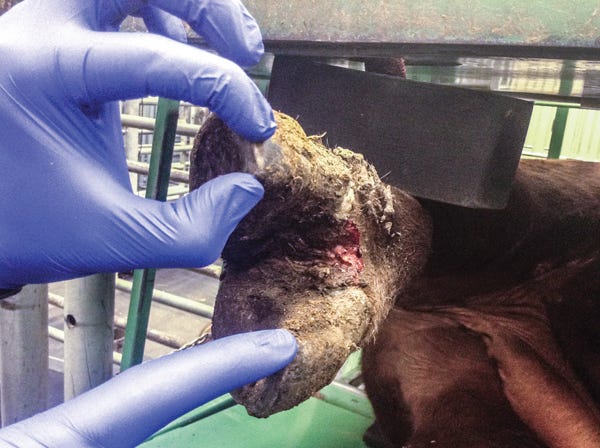
Strawberry foot rot is caused by a spirochete bacterium — Treponema spp. The lesion that appears with this type of lameness is a red, rough ulcer. It looks granular (like a strawberry), and doesn’t respond well to systemic antibiotics. Prevention is most recommended.
The detection of DD requires routine, systematic inspections by workers trained to recognize the disease at its various stages, report Dörte Döpfer and Arturo Gomez, University of Wisconsin School of Veterinary Medicine DVMs.
As DD is extremely difficult to eliminate, they recommend a focus on preventing new infections and decreasing the duration of acute cases. That means improved hygiene, reassessing stocking densities, avoiding grouping infected and healthy cattle, and screening cattle for lesions.
The duo’s research indicates that cattle supplemented with a specific combination of complexed and inorganic trace minerals experienced a 45.5% reduction in M2 lesions, compared to animals fed the control diet (of only inorganic trace minerals).
“Improving disease resistance and lowering the prevalence of DD in this way could be particularly advantageous in cattle that aren’t handled on a regular basis, such as pastured cattle and beef cattle in feedlots,” the researchers say.
You might also enjoy:
10 Ways To Have A Stress-Free Weaning Day
Effective Heifer Development Means Thinking Early & Long Term
BEEF Exclusive: Herd Expansion? BEEF Readers Say Its Go Time
15 ATVs and UTVs That Are New For 2014
Corn Projected In $2.70 To $3.20/Bu. Range Through 2020
ENTER NOW! 2014 BEEF Efficiency & Profit Contest
Nebraska Veterinarians Practice What They Preach At Family Feedlot
Is The Use Of Crossbred & Composite Bulls Is Catching On?
You May Also Like


.png?width=300&auto=webp&quality=80&disable=upscale)
